After Medicaid Coverage Loss, Insurance Campaign Launches In State

A record number of people are using services at the Missoula Food Bank and Community Center, and medical costs are the No. 2 reason they need help, according to the food bank director.
“Thirty percent are saying medical costs are the reason they are experiencing food insecurity today,” said Amy Allison-Thompson, executive director of the food bank; she said housing is the No. 1 reason.
April Seat, director of outreach for the Hope Rescue Mission, said some people don’t qualify for Medicaid, but it’s hard for them to afford insurance from the marketplace either because their paychecks are being garnished by as much as 80%.
“The majority of them are getting their paychecks garnished because of past medical bills,” Seat said.
Since last April, one-in-10 Montanans lost health insurance coverage through Medicaid or Healthy Montana Kids, or 132,000, according to Cover Montana. Coverage is pending for 41,000 people.
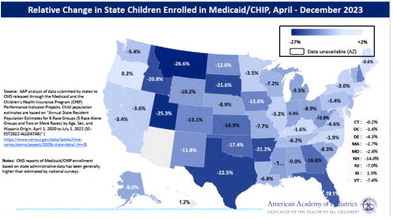
Montana also had the highest portion of children who lost coverage in the U.S. from April through December 2023, according to the American Academy of Pediatrics. It counted a 26.6% loss based on federal data from the Centers for Medicare and Medicaid Services.
On Thursday, some 20 state and community leaders in health care, education and social services met in Missoula at Partnership Health Center to launch a statewide “all-hands-on-deck” campaign to reregister Montanans for health insurance — the “Get Covered Again” campaign.
People lost coverage in the state process of determining whether people still qualified for Medicaid. The goal from Cover Montana, a program of the Montana Primary Care Association, is to reenroll people who still qualify for Medicaid and help others find an affordable plan on the Health Insurance Marketplace.
“Get Covered Again”
The campaign includes:
• Increased direct outreach to househlds who have lost Medicaid – Updated print materials and resources for partners – Medicaid application training and technical assistance – Clear referral pathways and complex care assistance “If you lost Medicaid or HMK (Healthy Montana Kids), you can still enroll in coverage through Health-Care.gov — you have until July 31, 2024,” said a Cover Montana flier.
To learn more about the roadmap to re-enrollment, visit www.mtpca.org/getcoveredagain or contact Rachel Pauli at rpauli@mtpca.org or 406-438-3410.
The loss of coverage means children who had starting making progress through therapy or other services couldn’t continue, said Kade Anderson, a licensed clinical professional counselor based in a public school.
“Unfortunately, in those situations, we would see that health care coverage — or lack of coverage — was what was guiding these treatment decisions versus the kids’ needs,” said Anderson, a behavioral health clinician with Partnership Health Center.
The lack of it has a trickle- down effect too, said Barbara Frank, with Missoula County Public Schools. It affects not just the 5-year-olds walking into the classroom without ever having seen a dentist, it affects their ability to read at third grade — which has impacts on their education through college and into their careers.
“Our community pays a higher cost in the end,” said Frank, P-12 academic and community services director.
Olivia Riutta, with Cover Montana, said more than 64% of people who lost coverage lost it for procedural reasons — or paperwork. Maybe they sent in documents a day late, she said.
“We actually don’t know if they qualify for Medicaid anymore,” said Riutta, director of special populations with the Montana Primary Care Association, which includes community health centers and urban Indian organizations.
But people are being told by the state that they are no longer covered, even if it’s not true, said SJ Howell, executive director of Montana Women Vote. And that’s a barrier for people in tough situations right out of the gate.
“That’s really confusing,” said Howell, also a state legislator from Missoula. “ … We actually need to start by saying, ‘It’s worth trying again. You may still be eligible.’” Riutta, who encouraged people and partner organizations to help identify those who need insurance, said some people may qualify for insurance from the marketplace, but some may qualify for Medicaid despite a letter from the state.
“We’re hearing that a ton, and it’s super concerning,” Riutta said of people who believe they are ineligible.
Jen Euell, head of the YWCA Missoula, said the insurance campaign may help people with housing during the long run, too, especially with the idea insurance experts could visit nonprofits in person. The 150 people housed at the shelter every night are among those most likely to have lost Medicaid, she said, and they stay an average of 3.5 months.
“So we have this unique window of opportunity to really connect them to all the resources that are going to ensure that they’re successful and aren’t back in our shelter in six months,” Euell said.
To directly reach people, Missoula Mayor Andrea Davis said a “guerrilla marketing campaign” might be helpful. She suggested pop-up tables at grocery stores, posters on cork boards, and information on the sides of vans that deliver services to people.
“Our communications have changed so, so drastically in the last several years as a society,” Davis said.
Most Montanans qualify for some form of financial help, according to Cover Montana.
“We have seen pretty staggering coverage loss,” Riutta said. “So we are really interested in what we can do across the state to get folks covered again.”

